Kelly Warner Law Firm Blames USA…
In what appears as a desperate attempt to defend multiple…
By – USA HeraldAaron Kelly Law Firm Resorts To…
Attorney Aaron Kelly and his law partner Daniel Warner are…
By – Jeff WattersonArizona Bar Opens Investigation on Attorney…
USA Herald recently reported on a developing story involving Attorneys…
By – Paul O'NealTurning the Page: Cassie Ventura Officially…
Cassie Ventura Confirms Departure from the U.S. Following Diddy Legal…
By – Tyler BrooksMystery in the Sewers: NYPD Investigates…
In recent weeks, New York City residents and law enforcement…
By – Tyler BrooksThe Guilty Verdict of Andrew Left:…
The recent federal court ruling finding prominent activist short-seller Andrew…
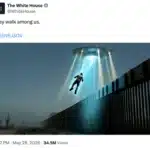
By – Tyler BrooksThe Pentagon’s ‘Flying Humanoid’: A Masterclass…
Pentagon UFO files human-shaped object, UAP declassification flying humanoid, military…
By – Tyler BrooksFBI Dismantles Sprawling Multi-State Drug Rings…
MARTINSBURG, WV — In a major coordinated federal and local…
By – Tyler BrooksDeep Divide: Inside the Unprecedented Feud…
A major institutional crisis has surfaced at the highest echelons…
By – Tyler BrooksOperation Iron Pursuit Leads to Hundreds…
Operation Iron Pursuit continues to generate significant results in the…
By – Jackie AllenJosh Duggar Appeal Denied as Convicted…
Josh Duggar remains behind bars after a federal judge denied…
By – Jackie AllenFederal Judge Lets ’86 47′ Flag…
An Obama-appointed judge just ruled a political group can keep…
By – Samuel LopezSouth Carolina Jury Clears Store Owner…
A South Carolina courtroom erupted with emotion Monday after a…
By – Tyler BrooksSleeping Dog Documentary Chronicles Jeremy Corbell’s…
The new documentary Sleeping Dog arrives at a pivotal moment…
By – Jackie AllenKendall Jenner, Jacob Elordi and the…
I’ve been writing about royals and celebrities for 20 years.…
By – Nathan KayRare Blue Micromoon Lights Up the…
Skywatchers are in for a unique celestial event as a…
By – Jackie AllenMurder-for-hire Ends with Life Sentence for…
A shocking Murder-for-hire case that spanned multiple states has concluded…
By – Jackie AllenFrank Lloyd Wright and the Taliesin…
In The Killer and Frank Lloyd Wright, veteran true-crime author…
By – Jackie AllenHollywood at a Crossroads: Spencer Pratt…
Los Angeles has its primary election this Tuesday, and the…
By – Jackie AllenHayden Panettiere has a Memoir About…
Hayden Panettiere is revealing the emotional toll of growing up…
By – Jackie AllenBlue Origin Rocket Explodes in Massive…
Blue Origin suffered a major setback Thursday night when one…
By – Jackie AllenBlue Origin Rocket Explodes in Massive…
Blue Origin suffered a major setback Thursday night when one…
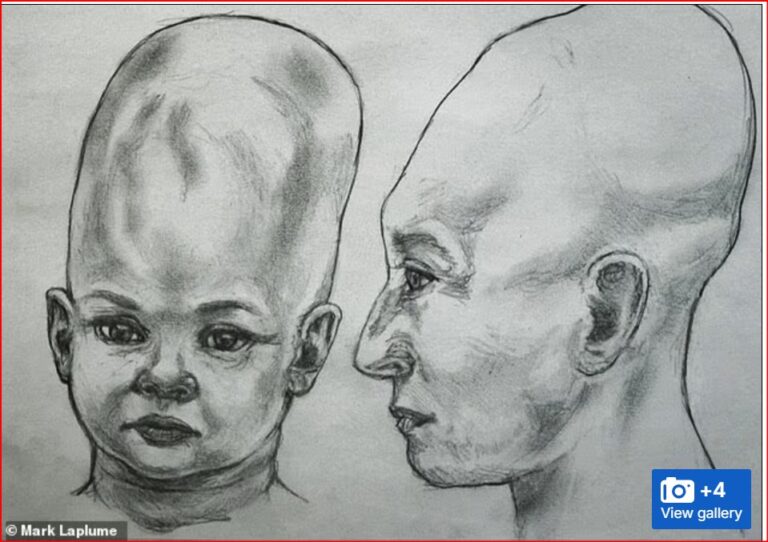
By – Jackie AllenAlien Coneheads: New DNA Study Doesn’t…
The mystery surrounding the so-called Alien Coneheads of Peru has…
By – Jackie AllenTrump’s Alien.gov Reveal Turns Into Immigration…
INSIDE THIS REPORT What millions thought would be a historic…
By – Samuel LopezTrump’s UFO files reveal mysterious flying…
The newly released UFO Files from the Trump administration have…
By – Jackie AllenWho’s Lying? E. Jean Carroll Faces…
Author and columnist E. Jean Carroll is once again at…
By – Jackie AllenSuper El Niño: Will 2026 be…
Scientists across the globe are increasingly warning that a potential…
By – Jackie AllenTitle: 2026 Midterm Primaries: Key Takeaways…
Discover the crucial results of the June 2, 2026 midterm…
By – Tyler BrooksBakersfield Bomb Threat Standoff: FBI Assumes…
BAKERSFIELD, California — A massive multi-agency police response completely locked…
By – Tyler BrooksSabrina Carpenter Granted Restraining Order Following…
Citing “severe emotional distress,” the American pop star has successfully…
By – Tyler BrooksThe Diddy Fallout: Cassie Fights Back…
As Sean “Diddy” Combs serves time behind bars, the shockwaves…
By – Tyler BrooksArcher Aviation: The eVTOL Takeoff Facing…
Strategic Analysis — June 2026 The electric vertical takeoff and…
By – Tyler BrooksFrom a Casual Night Out to…
It Doesn’t Happen Here’: Quiet Suburb Left Shattered After Fatal…
By – Tyler BrooksNew Pill Doubles Survival for Pancreatic…
Pancreatic cancer pill doubles life to 13 months By Tyler…
By – Tyler BrooksFDA warns public as cookie firm…
FDA warns public as cookie firm rejects urgent recall request…
By – Tyler BrooksTrump orders CDC to slash childhood…
Trump orders CDC to slash childhood vaccines from 17 to…
By – Tyler BrooksUSDA warns Americans over Salmonella in…
USDA warns Americans over Salmonella in meat products By Tylor…
By – Tyler BrooksGKN Aerospace’s Biggest Battle May Not…
By Samuel López | USA Herald The immediate danger of…
By – Samuel LopezGarden Grove Chemical Crisis Sparks Class…
By Samuel López | USA Herald A full-scale legal and…
By – Samuel LopezWembanyama in Tears: Spurs Dethrone Thunder…
Spurs dethrone Thunder in epic Game 7 road victory By…
By – Tyler BrooksSupreme Court signals 27 states could…
Supreme Court signals 27 states could ban trans female athletes…
By – Tyler BrooksMauricio Pochettino sounds alarm on Chris…
Mauricio Pochettino sounds alarm on Chris Richards injury By Tylor…
By – Tyler BrooksUSMNT star Chris Richards tears two…
USMNT star Chris Richards tears two ankle ligaments By Tylor…
By – Tyler Brooks“Money” Mayweather Tucks Tail: $100 Million…
Floyd Mayweather has beaten every opponent who ever climbed into…
By – Samuel LopezMackenzie Shirilla Sent Text Messages to…
Mackenzie Shirilla is once again at the center of public…
By – Jackie AllenNo posts found.
No posts found.





































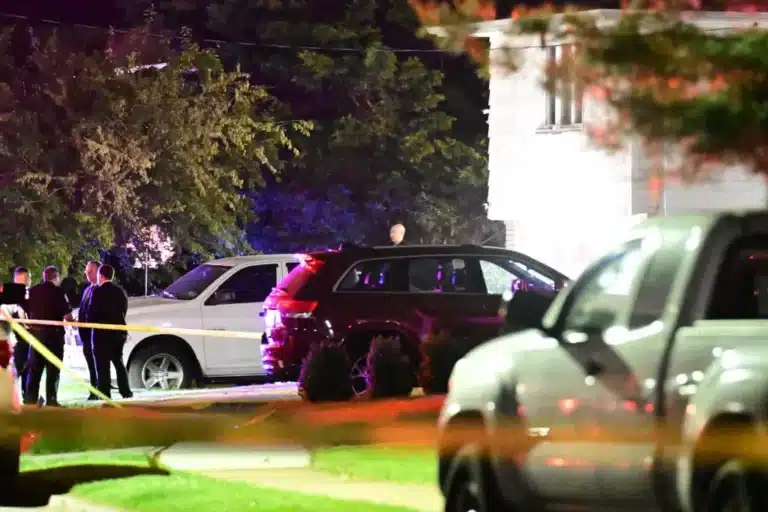













For the reason that the admin of this site is working, no uncertainty very quickly it will be renowned, due to its quality contents.